Special Message
“Never Avoid Your Sex Problems Other Wise Your Partner Can Avoid You.”
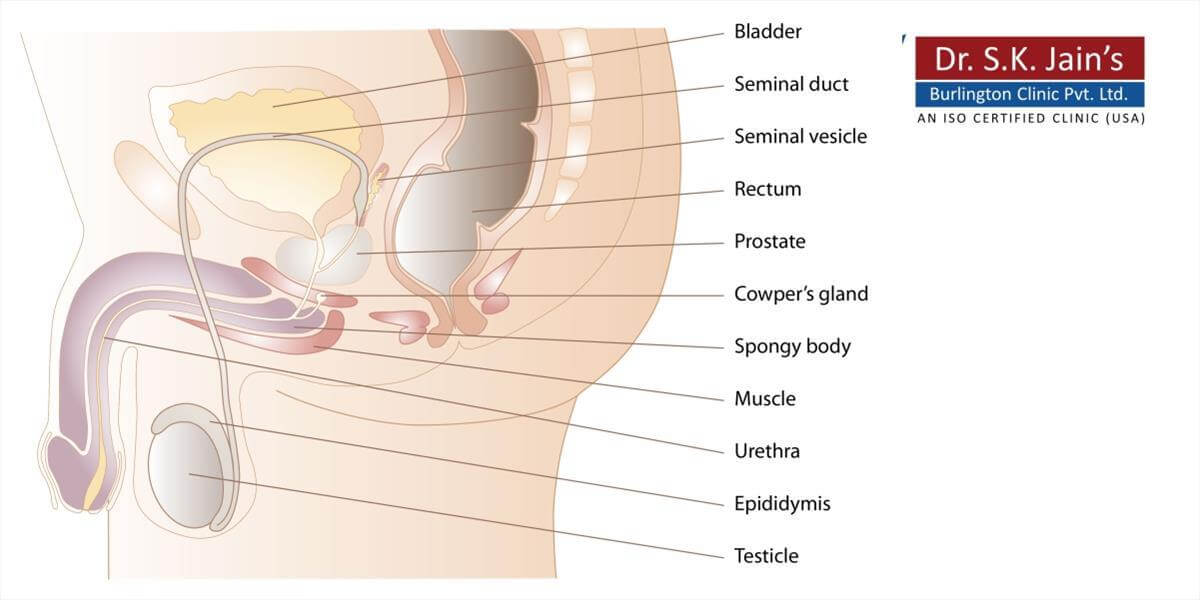
Unlike the female, whose sex organs are located entirely within the pelvis, the male has reproductive organs, or genitals, that are both inside and outside the pelvis. The male genitals include:
In a guy who has reached sexual maturity, the two testicles, or testes, produce and store millions of tiny sperm cells. The testicles are oval-shaped and grow to be about 2 inches (5 centimeters) in length and 1 inch (3 centimeters) in diameter. The testicles are also part of the endocrine system because they produce hormones, including testosterone. Testosterone is a major part of puberty in boys, and as a guy makes his way through puberty, his testicles produce more and more of it. Testosterone is the hormone that causes boys to develop deeper voices, bigger muscles, and body and facial hair, and it also stimulates the production of sperm.
Alongside the testicles are the epididymis and the vas deferens, which make up the duct system of the male reproductive organs. The vas deferens is a muscular tube that passes upward alongside the testicles and transports the sperm-containing fluid called semen. The epididymis is a set of coiled tubes (one for each testicle) that connects to the vas deferens.
The epididymis and the testicles hang in a pouch-like structure outside the pelvis called the scrotum. This bag of skin helps to regulate the temperature of testicles, which need to be kept cooler than body temperature to produce sperm. The scrotum changes size to maintain the right temperature. When the body is cold, the scrotum shrinks and becomes tighter to hold in body heat. When it's warm, the scrotum becomes larger and more floppy to get rid of extra heat. This happens without a guy ever having to think about it. The brain and the nervous system give the scrotum the cue to change size.
The accessory glands, including the seminal vesicles and the prostate gland, provide fluids that lubricate the duct system and nourish the sperm. The seminal vesicles are sac-like structures attached to the vas deferens to the side of the bladder. The prostate gland, which produces some of the parts of semen, surrounds the ejaculatory ducts at the base of the urethra, just below the bladder. The urethra is the channel that carries the semen to the outside of the body through the penis. The urethra is also part of the urinary system because it is also the channel through which urine passes as it leaves the bladder and exits the body.
The penis is actually made up of two parts: the shaft and the glans. The shaft is the main part of the penis and the glans is the tip (sometimes called the head). At the end of the glans is a small slit or opening, which is where semen and urine exit the body through the urethra. The inside of the penis is made of a spongy tissue that can expand and contract.
All boys are born with a foreskin, a fold of skin at the end of the penis covering the glans. Some boys are circumcised, which means that a doctor or clergy member cuts away the foreskin. Circumcision is usually performed during a baby boy's first few days of life. Although circumcision is not medically necessary, parents who choose to have their children circumcised often do so based on religious beliefs, concerns about hygiene, or cultural or social reasons. Boys who have circumcised penises and those who don't are no different: All penises work and feel the same, regardless of whether the foreskin has been removed.
The male reproductive system creates sperm that is manufactured in the seminiferous tubules within each testicle. The head of the sperm contains the DNA, which when combined with the egg's DNA, will create a new individual. The tip of the sperm head is the portion called the acrosome, which enables the sperm to penetrate the egg. The midpiece contains the mitochondria which supplies the energy the tail needs to move. The tail moves with whip-like movements back and forth to propel the sperm towards the egg. The sperm have to reach the uterus and the fallopian tube in order to fertilize a woman's egg.
Male fertility depends on the proper function of a complex system of organs and hormones:
· The process begins in the area of the brain called the hypothalamus-pituitary axis, a system of glands, hormones, and chemical messengers called neurotransmitters, all of which are critical for reproduction.
· The first step in fertility is the production of gonadotropin-releasing hormone (GnRH) in the hypothalamus, which prompts the pituitary gland to manufacture follicle-stimulating hormone (FSH) and luteinizing hormone (LH).
· FSH maintains sperm production, and LH stimulates the production of the male hormone testosterone.
· Both sperm and testosterone production occurs in the two testicles, or testes, which are contained in the scrotal sac (the scrotum). (This sac develops on the outside of the body because normal body temperature is too high to allow sperm production.)
The male reproductive structures include the penis, the scrotum, the seminal vesicles, and the prostate.
Sperm are manufactured in several hundred microscopic tubes, known as seminiferous tubules, which make-up most of the testicles.
Surrounding these tubules are clumps of tissue containing so-called Leydig cells. Here, testosterone is manufactured.
Sperm Development. The life cycle of sperm consists of a remarkable journey that depends on hormonal signals combined with a mechanical process. It takes about 74 days:
· Sperm begin partially embedded in nurturing Sertoli cells, which are located in the lower parts of the seminiferous tubules.
· As they mature and move along, they are stored in the upper part of the tubules. Young sperm cells are known as spermatids.
· When the sperm has completed the development of its head and tail, it is released from the cell into the epididymis. This remarkable C-shaped tube is 1/300 of an inch in diameter and about 20 feet long. It loops back and forth on itself within a space that is only about one and a half inches long. The sperm's journey through the epididymis takes about 3 weeks.
· The fluid in which the sperm is transported contains sugar in the form of fructose, which provides energy as the sperm matures. In the early stages of its passage, the sperm cannot swim in a forward direction and can only vibrate its tail weakly. By the time the sperm reaches the end of the epididymis, however, it is mature and looks like a microscopic squirming tadpole.
· At maturity, each healthy sperm consists of a head that contains the man's genetic material, his DNA, and a tail that lashes back and forth at great speed to propel the head forward at about four times its own length every second.The ability of a sperm to move forward rapidly and straight is probably the most significant determinant of male fertility.
Ejaculation. When a man experiences sexual excitement, nerves stimulate the muscles in the epididymis to contract, which forces the sperm out through the penis:
· After being produced in the testicle, the sperm first pass through the epididymis and then into one of two rigid and wire-like muscular channels, called the vasa deferentia. (A single channel is called a vas deferens.)
· Muscle contractions in the vas deferens from sexual activity propel the sperm along past the seminal vesicles. These are clusters of tissue that contribute fluid, called seminal fluid, to the sperm. The vas deferens also collects fluid from the nearby prostate gland. This mixture of various fluids and sperm is the semen.
· Each vas deferens then joins together to form the ejaculatory duct. This duct, which now contains the sperm-containing semen, passes down through the urethra. (The urethra is the same channel in the penis through which a man urinates, but during orgasm, muscles close off the bladder so that urine cannot enter the urethra.)
· The semen is forced through the urethra during ejaculation, the final stage of orgasm when the sperm is literally shot out of the penis.
Pathway of sperm
Click the icon to see an image of the vas deferens.
Semen. In addition to providing the fluid that transports the sperm, semen also has other benefits:
· It provides a very short-lived alkaline environment to protect sperm from the harsh acidity of the female vagina. (If the sperm do not reach the woman's cervix within several hours, the semen itself becomes toxic to sperm and they die.)
· It contains a gelatin-like substance that prevents it from draining from the vagina too quickly.
· It contains sugar in the form of fructose to provide instant energy for sperm locomotion.
The Path to the Egg. The sperm's passage to the egg is a difficult journey.
· Usually about 100 - 300 million sperm are delivered into the ejaculate at any given time. Even under normal conditions, however only about 15% of these millions of sperm are sound enough to fertilize an egg.
· To compound the problem, after the stress of ejaculation, only about 400 sperm survive the orgasm to complete the journey.
· Out of this number, a mere 40 or so sperm survive the toxicity of the semen and the hostile environment of the vagina to reach the vicinity of the egg. Normally, the cervical mucus forms an impenetrable barrier to sperm. However, when a woman ovulates (releases her egg, the oocyte), the mucus lining thins to allow sperm penetration.
· Sperm that manage to reach the mucus lining in the woman's cervix (the lower part of her uterus) must survive about four more days to reach the woman's fallopian tubes. (Here, the egg is positioned for fertilization for only 12 hours each month.)
· The few remaining sperm that penetrate the cervical mucus and are able to reach the fallopian tubes becomecapacitated.
· Capacitation is a one-time explosion of energy that completes the sperm's journey. It boosts the motion of the sperm and triggers the actions of the acrosome, a membrane that covers the head of the sperm and resembles a warhead. The acrosome is dissolved, and enzymes contained within it are released to allow the sperm to drill a hole through the tough outer coating of the egg.
· In the end, only one sperm gets through to fertilize the egg.
ANATOMY OF PENIS:-
What the Male Reproductive System Does
The male sex organs work together to produce and release semen into the reproductive system of the female during sexual intercourse. The male reproductive system also produces sex hormones, which help a boy develop into a sexually mature man during puberty.
When a baby boy is born, he has all the parts of his reproductive system in place, but it isn't until puberty that he is able to reproduce. When puberty begins, usually between the ages of 10 and 14, the pituitary gland — which is located near the brain — secretes hormones that stimulate the testicles to produce testosterone. The production of testosterone brings about many physical changes. Although the timing of these changes is different for every guy, the stages of puberty generally follow a set sequence.
During the first stage of male puberty, the scrotum and testes grow larger.
Next, the penis becomes longer, and the seminal vesicles and prostate gland grow.
Hair begins to appear in the pubic area and later it grows on the face and underarms. During this time, a male's voice also deepens.
Boys also undergo a growth spurt during puberty as they reach their adult height and weight.
A male who has reached puberty will produce millions of sperm cells every day. Each sperm is extremely small: only 1/600 of an inch (0.05 millimeters long). Sperm develop in the testicles within a system of tiny tubes called the seminiferous tubules. At birth, these tubules contain simple round cells, but during puberty, testosterone and other hormones cause these cells to transform into sperm cells. The cells divide and change until they have a head and short tail, like tadpoles. The head contains genetic material (genes). The sperm use their tails to push themselves into the epididymis, where they complete their development. It takes sperm about 4 to 6 weeks to travel through the epididymis.
The sperm then move to the vas deferens, or sperm duct. The seminal vesicles and prostate gland produce a whitish fluid called seminal fluid, which mixes with sperm to form semen when a male is sexually stimulated. The penis, which usually hangs limp, becomes hard when a male is sexually excited. Tissues in the penis fill with blood and it becomes stiff and erect (an erection). The rigidity of the erect penis makes it easier to insert into the female's vagina during sexual intercourse. When the erect penis is stimulated, muscles around the reproductive organs contract and force the semen through the duct system and urethra. Semen is pushed out of the male's body through his urethra — this process is called ejaculation. Each time a guy ejaculates, it can contain up to 500 million sperm.
When the male ejaculates during intercourse, semen is deposited into the female's vagina. From the vagina the sperm make their way up through the cervix and move through the uterus with help from uterine contractions. If a mature egg is in one of the female's fallopian tubes, a single sperm may penetrate it, and fertilization, or conception, occurs.
This fertilized egg is now called a zygote and contains 46 chromosomes — half from the egg and half from the sperm. The genetic material from the male and female has combined so that a new individual can be created. The zygote divides again and again as it grows in the female's uterus, maturing over the course of the pregnancy into an embryo, a fetus, and finally a newborn baby.